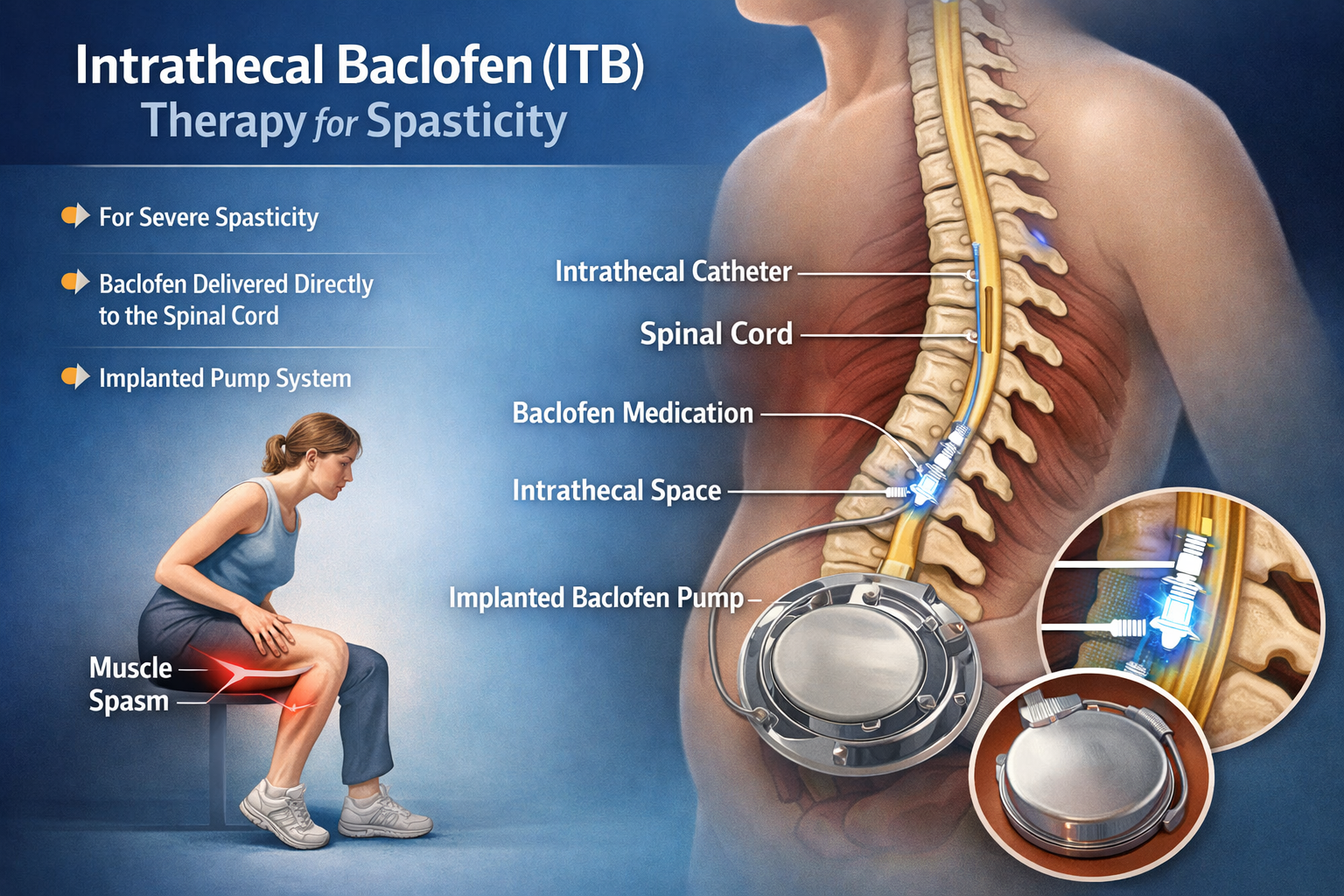
Intrathecal Baclofen (ITB) therapy is an advanced treatment used to manage severe spasticity—an abnormal increase in muscle stiffness and tightness that interferes with normal movement, posture, and daily activities. Spasticity often occurs due to neurological conditions affecting the brain or spinal cord, where the communication between nerves and muscles becomes disrupted. ITB therapy works by delivering baclofen, a muscle relaxant medication, directly into the spinal fluid through a small implanted pump.
Unlike oral medications that circulate through the entire body and may cause systemic side effects, intrathecal delivery allows the drug to act precisely where it is needed—the spinal cord. This targeted approach provides effective muscle relaxation with much lower doses of medication. ITB therapy is commonly recommended for patients whose spasticity is severe, disabling, and not adequately controlled with conventional treatments such as oral medications or physiotherapy.
Spasticity develops when there is damage or dysfunction in the parts of the brain or spinal cord responsible for controlling voluntary movement and muscle tone. When these pathways are disrupted, the normal signals that regulate muscle relaxation are impaired, resulting in continuous muscle contraction and stiffness.
Several neurological conditions can lead to severe spasticity. These include cerebral palsy, spinal cord injuries, traumatic brain injuries, multiple sclerosis, stroke, and certain neurodegenerative disorders. In many of these conditions, the injury interrupts the normal inhibitory signals from the brain to the spinal cord, causing exaggerated reflexes and muscle tightness. Over time, untreated spasticity can lead to pain, joint deformities, contractures, and difficulty performing routine activities.
The symptoms of spasticity vary depending on the severity of the underlying neurological condition and the muscles involved. Patients commonly experience persistent muscle stiffness, tightness, and involuntary muscle spasms that make movement difficult. The muscles may feel rigid, and simple tasks such as walking, sitting, or maintaining posture can become challenging.
In severe cases, spasticity may cause painful muscle contractions, abnormal limb positions, and reduced range of motion in joints. Patients may also experience fatigue, sleep disturbances, and difficulty with personal care activities. Over time, prolonged muscle tightness can lead to joint stiffness, contractures, and secondary complications that significantly impact quality of life.
The diagnosis of spasticity and the evaluation for Intrathecal Baclofen therapy involve a detailed clinical assessment by a neurosurgeon or neurologist. The evaluation begins with a thorough medical history and physical examination to assess muscle tone, reflexes, strength, and functional limitations. The doctor carefully evaluates how spasticity affects mobility, posture, daily activities, and overall quality of life.
Additional diagnostic tests may be performed to understand the underlying neurological condition. These may include imaging studies such as MRI of the brain or spinal cord, nerve conduction studies, or other neurological assessments. Before proceeding with permanent pump implantation, many patients undergo a baclofen trial, where a small dose of the medication is injected into the spinal fluid to evaluate how effectively it reduces spasticity.
Management of spasticity usually begins with conservative treatments such as physical therapy, stretching exercises, and oral medications that help relax muscles. While these approaches can provide relief for mild to moderate spasticity, some patients with severe neurological conditions may not respond adequately to them or may experience significant side effects from high medication doses.
Intrathecal Baclofen therapy offers a more targeted and effective treatment for such cases. During the procedure, a small programmable pump is surgically implanted under the skin of the abdomen. This pump delivers controlled doses of baclofen through a thin catheter placed into the intrathecal space around the spinal cord. The dosage can be precisely adjusted based on the patient’s symptoms, allowing personalized and long-term control of spasticity. By directly delivering medication to the spinal cord, ITB therapy significantly reduces muscle stiffness, improves comfort, and enhances mobility and daily functioning.
After the implantation of the intrathecal baclofen pump, patients require regular follow-up visits to monitor treatment effectiveness and adjust medication doses if necessary. The pump is programmable, allowing physicians to fine-tune the amount of medication delivered according to the patient’s response and functional goals.
Patients also need periodic pump refills, which are performed through a simple outpatient procedure using a needle to inject medication into the pump reservoir. Rehabilitation, physiotherapy, and guided exercises remain important components of recovery, helping patients improve flexibility, strength, and mobility as muscle stiffness decreases. With appropriate follow-up care, many patients experience long-term improvement in comfort and quality of life.
As with any surgical procedure, Intrathecal Baclofen therapy carries certain risks, although serious complications are relatively uncommon when performed by experienced specialists. Possible risks include infection at the surgical site, catheter malfunction, pump-related issues, or leakage of spinal fluid. In some cases, improper medication dosing may lead to symptoms such as excessive weakness, drowsiness, or dizziness.
Another important consideration is baclofen withdrawal, which can occur if the pump stops delivering medication unexpectedly. This is a rare but serious situation that requires immediate medical attention. Regular monitoring and timely pump maintenance significantly reduce the likelihood of such complications.
Medical evaluation is recommended when muscle stiffness, spasms, or tightness begin to interfere with movement, comfort, or daily activities. Individuals with neurological conditions such as cerebral palsy, spinal cord injury, or multiple sclerosis who experience worsening spasticity despite medications or therapy should consult a neurosurgeon or specialist.
Early assessment allows doctors to determine the severity of spasticity and recommend appropriate treatment options. For patients with severe or disabling symptoms, Intrathecal Baclofen therapy may provide effective and long-term relief, improving mobility, comfort, and overall quality of life. Timely consultation with a qualified neurosurgeon can help determine whether this advanced treatment option is suitable for a patient’s specific condition.
“Dr. Raghu Samala provides comprehensive diagnosis and advanced treatment for a wide range of neurological diseases and disorders, ensuring personalized and compassionate care for every patient.”
