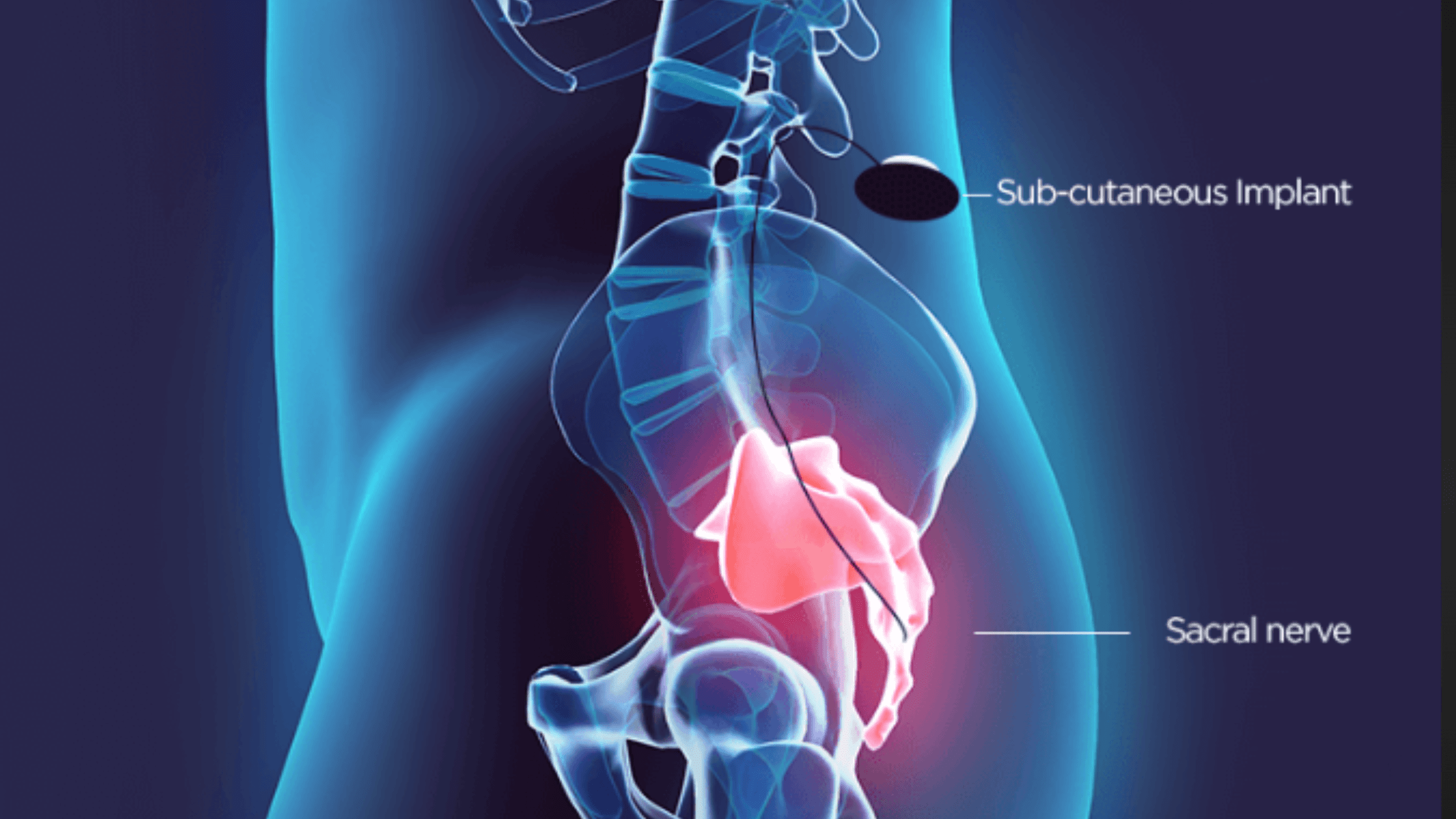
Sacral Nerve Modulation (SNM), also known as sacral nerve stimulation, is a minimally invasive therapy used to treat certain bladder and bowel control disorders. The treatment works by sending mild electrical impulses to the sacral nerves, which are located in the lower part of the spine and play an important role in regulating bladder, bowel, and pelvic floor function. When these nerves do not communicate properly with the brain, it can lead to problems such as urinary urgency, urinary incontinence, or fecal incontinence. Sacral nerve modulation helps restore more normal communication between the brain and the pelvic organs, improving control and reducing symptoms. The therapy usually begins with a temporary test phase to determine whether the patient responds well before a permanent device is implanted.
Sacral nerve modulation is typically recommended for patients whose bladder or bowel control problems do not improve with medications, lifestyle changes, or other non-surgical treatments. The underlying causes of these conditions often involve disrupted nerve signals between the brain and pelvic organs. Conditions such as overactive bladder, chronic urinary retention, and fecal incontinence may arise due to nerve dysfunction, pelvic floor disorders, spinal conditions, childbirth-related injuries, or previous pelvic surgeries. In some cases, neurological conditions affecting nerve pathways can also interfere with normal bladder and bowel control.
Patients who may benefit from sacral nerve modulation often experience persistent symptoms related to bladder or bowel control. Common symptoms include frequent and sudden urges to urinate, involuntary leakage of urine, difficulty emptying the bladder completely, and repeated nighttime urination. Some individuals may also experience loss of bowel control, accidental stool leakage, or a constant feeling of urgency related to bowel movements. These symptoms can significantly impact daily activities, sleep, work, and social life, often leading to discomfort, embarrassment, and reduced quality of life.
Diagnosis begins with a detailed medical history and physical examination to understand the nature and severity of the patient’s symptoms. Doctors may recommend several diagnostic tests to evaluate bladder and bowel function. These tests may include urodynamic studies to assess bladder activity, ultrasound imaging to examine the urinary system, and specialized tests to measure pelvic floor function. In some cases, additional neurological assessments may be required to identify possible nerve-related causes. If conservative treatments fail, a temporary sacral nerve modulation trial may be performed to determine whether electrical stimulation improves symptoms before considering permanent implantation.
Sacral nerve modulation is considered when other treatments such as medications, pelvic floor exercises, behavioral therapy, or minimally invasive procedures do not provide adequate relief. The therapy involves placing a thin electrode near the sacral nerves through a small incision in the lower back. This electrode is connected to a small device that delivers gentle electrical pulses to regulate nerve activity. Initially, a temporary external device is used during the testing phase to evaluate symptom improvement. If the trial period shows significant benefit, a small permanent stimulator is implanted under the skin, typically in the upper buttock area. The device can be adjusted to provide optimal stimulation levels based on the patient’s needs.
After the procedure, patients are usually able to return to normal daily activities within a short period, although heavy physical activity may be restricted for a few weeks. Regular follow-up visits are important to monitor the performance of the device and adjust stimulation settings if needed. Patients are also advised to maintain healthy bladder and bowel habits, follow any recommended pelvic floor rehabilitation programs, and report any unusual symptoms to their doctor promptly. Proper care helps ensure long-term effectiveness and comfort with the device.
Sacral nerve modulation is generally a safe and well-tolerated procedure, but some risks may occur. Possible complications include mild discomfort at the implant site, infection, temporary pain near the electrode, or movement of the device or leads. In rare cases, the device may require reprogramming or repositioning if symptoms return or if stimulation becomes uncomfortable. With proper surgical technique and regular monitoring, most patients experience significant symptom improvement with minimal complications.
Patients should seek medical advice if they experience ongoing bladder or bowel control problems that interfere with daily life. Frequent urination, sudden urgency, leakage of urine or stool, or difficulty emptying the bladder are signs that should not be ignored. If these symptoms persist despite lifestyle changes or medications, consultation with a specialist can help determine whether advanced treatments such as sacral nerve modulation may be appropriate. Early evaluation can lead to effective management and improved quality of life.