Parkinson’s disease lesioning is a specialized neurosurgical procedure used to manage certain symptoms of Parkinson’s disease when medications no longer provide adequate relief. Parkinson’s disease is a progressive neurological disorder that affects movement, leading to symptoms such as tremors, stiffness, slowed movement, and difficulties with balance and coordination. Lesioning procedures work by creating a small, precisely targeted lesion in specific areas of the brain that are responsible for abnormal movement signals. By interrupting these faulty signals, the procedure helps reduce symptoms such as tremors, rigidity, and involuntary movements. Although modern treatments like deep brain stimulation are commonly used, lesioning procedures remain an effective option for selected patients, particularly those who may not be suitable candidates for device-based therapies.
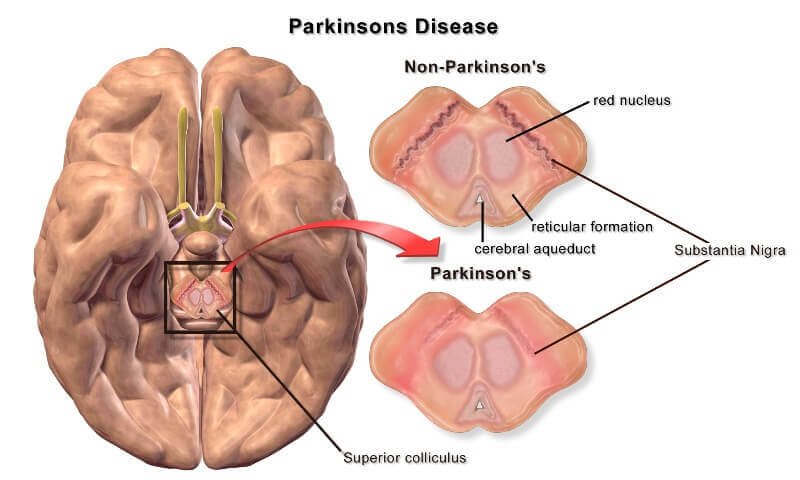
Parkinson’s disease occurs due to the gradual loss of dopamine-producing nerve cells in a region of the brain called the substantia nigra. Dopamine is a chemical messenger that plays a key role in controlling smooth and coordinated muscle movements. As dopamine levels decrease, abnormal electrical activity develops in certain brain circuits that regulate movement. This disruption leads to the characteristic motor symptoms of Parkinson’s disease. Lesioning procedures target specific structures within these circuits, such as the thalamus, globus pallidus, or subthalamic region, to reduce the abnormal signaling responsible for tremors and movement difficulties.
Patients with Parkinson’s disease often experience a range of movement-related symptoms that gradually worsen over time. The most common symptom is tremor, typically starting in one hand or limb and becoming more noticeable during rest. Other symptoms include muscle stiffness, slowed movement (bradykinesia), and difficulty maintaining balance or posture. As the condition progresses, patients may also experience reduced facial expression, softer speech, and difficulty performing everyday tasks such as writing, walking, or dressing. In some cases, involuntary movements caused by long-term medication use may also develop. When these symptoms become difficult to control with medication alone, surgical treatments such as lesioning may be considered.
The diagnosis of Parkinson’s disease is primarily based on a detailed clinical evaluation by a neurologist or neurosurgeon. The assessment includes a thorough review of symptoms, medical history, and a neurological examination to evaluate movement, muscle tone, reflexes, and coordination. Imaging studies such as MRI or CT scans may be performed to rule out other neurological conditions that could cause similar symptoms. For patients being considered for lesioning surgery, additional evaluations may be conducted to assess disease severity, medication response, and overall health status to determine whether the procedure is appropriate.
Treatment for Parkinson’s disease usually begins with medications that help increase or mimic dopamine in the brain, which can significantly improve symptoms in the early stages of the disease. Over time, however, medication effectiveness may decline or lead to complications such as involuntary movements. In such cases, surgical treatments may be recommended. Parkinson’s disease lesioning involves creating a small targeted lesion in a specific brain structure responsible for abnormal motor activity. Common procedures include thalamotomy for tremor control and pallidotomy for reducing rigidity and involuntary movements. The procedure is typically performed using advanced imaging and stereotactic techniques that allow the surgeon to precisely target the affected area while minimizing damage to surrounding brain tissue.
After lesioning surgery, patients are closely monitored during the recovery period to assess neurological function and symptom improvement. Most individuals experience a gradual reduction in tremors or stiffness following the procedure. Physical therapy and rehabilitation may be recommended to help improve mobility, balance, and strength. Patients will also continue regular follow-up visits with their neurologist or neurosurgeon to monitor disease progression and adjust medications if necessary. Ongoing care plays an important role in maintaining functional independence and overall quality of life.
As with any brain surgery, Parkinson’s disease lesioning carries certain risks. Potential complications may include bleeding in the brain, infection, temporary or permanent weakness, speech difficulties, or problems with coordination. In rare cases, unintended effects on nearby brain structures may occur. However, advances in imaging technology and surgical techniques have significantly improved the safety and precision of these procedures. Careful patient selection and experienced surgical teams help minimize the likelihood of complications.
Individuals experiencing symptoms such as persistent tremors, slowed movement, muscle stiffness, or balance problems should seek medical evaluation for proper diagnosis and treatment. Patients with Parkinson’s disease who notice worsening symptoms despite medication or who develop significant side effects from long-term drug therapy may benefit from consultation with a neurosurgical specialist. Early evaluation and appropriate treatment planning can help manage symptoms more effectively and improve the patient’s quality of life.